Why hire an ICU physician when you can hire a midlevel instead?
💬 0 comments
Is the kind of ICU you would want yourself or your loved one to be a patient in?
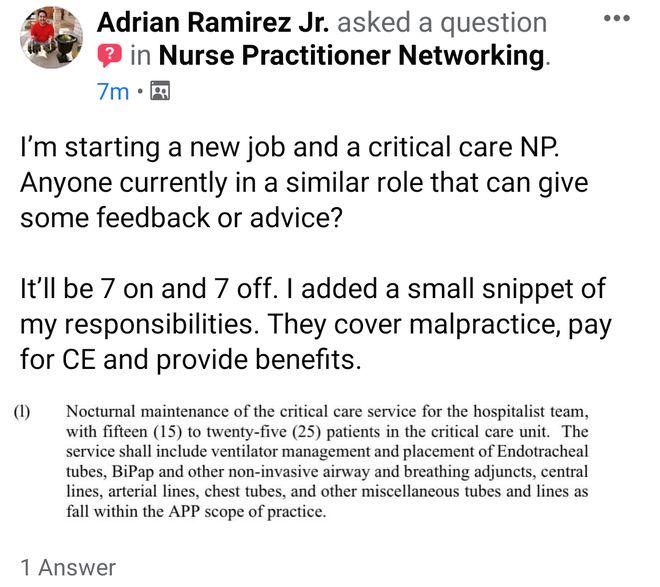
If this is just a "small snippet of [his] responsibilities", we're truly afraid to see what the entire scope is. One NP, in charge of 15-25 critical patients, doing everything from ventilator management to both invasive and non-invasive ventilation, and line and tube placement? Because clearly, these are all free simple and straightforward things to do. Do years of residency and critical care fellowship training mean nothing to the people hiring for this hospital? Who is this nurse practitioner going to call when shit inevitably hits the fan? What are they going to do when the morbidly obese, severe COPD, ASA class IV patient who barely has a neck decompensates on BiPAP and can't be intubated using whatever rudimentary endotracheal intubation skills they might have learned in their several-hundred-hour NP curriculum? Can they do a nasal intubation? Can they do a retrograde intubation? Can they do an emergent trach when all else fails? Who are they going to call when the patient's blood pressure is 60/40 and for whatever reason, they can't get access for a central line? These are the kinds of unpleasant questions with unpleasant answers that would not need to be asked if this hospital decided to stop pinching pennies and hire an attending physician with proper training in critical care medicine. Even a second-year emergency medicine or anesthesiology resident would be a vastly better choice, as one could expect them to be reasonably competent in the basic, bread-and-butter procedures of the ICU.

Certainly, both of these options would possess infinitesimally more training and experience than a newly minted midlevel who, according to the post above, just passed their FNP exam in December 2020. I wouldn't even trust an FNP to independently run a primary care clinic, and now, this hospital wants a fresh FNP graduate to managing one to two dozen ICU patients, establishing definitive airways, managing ventilator settings, and placing chest tubes? God help us all.