About
MidlevelWTF aims to aggregate and publish content that documents and exposes examples of midlevel malpractice, misconduct, and medical ignorance in order to show why allowing midlevels to practice independently without physician supervision is bad for patients and bad for doctors.
What are midlevels, and why do they matter?
Title 21 of the United States Code of Federal Regulations, Section 1300.01(b28), defines a mid-level practitioner as an individual practitioner, other than a physician, dentist, veterinarian, or podiatrist, examples of which include, but are not limited to, health care providers such as nurse practitioners, nurse midwives, nurse anesthetists, clinical nurse specialists and physician assistants who are authorized to dispense controlled substances by the state in which they practice.
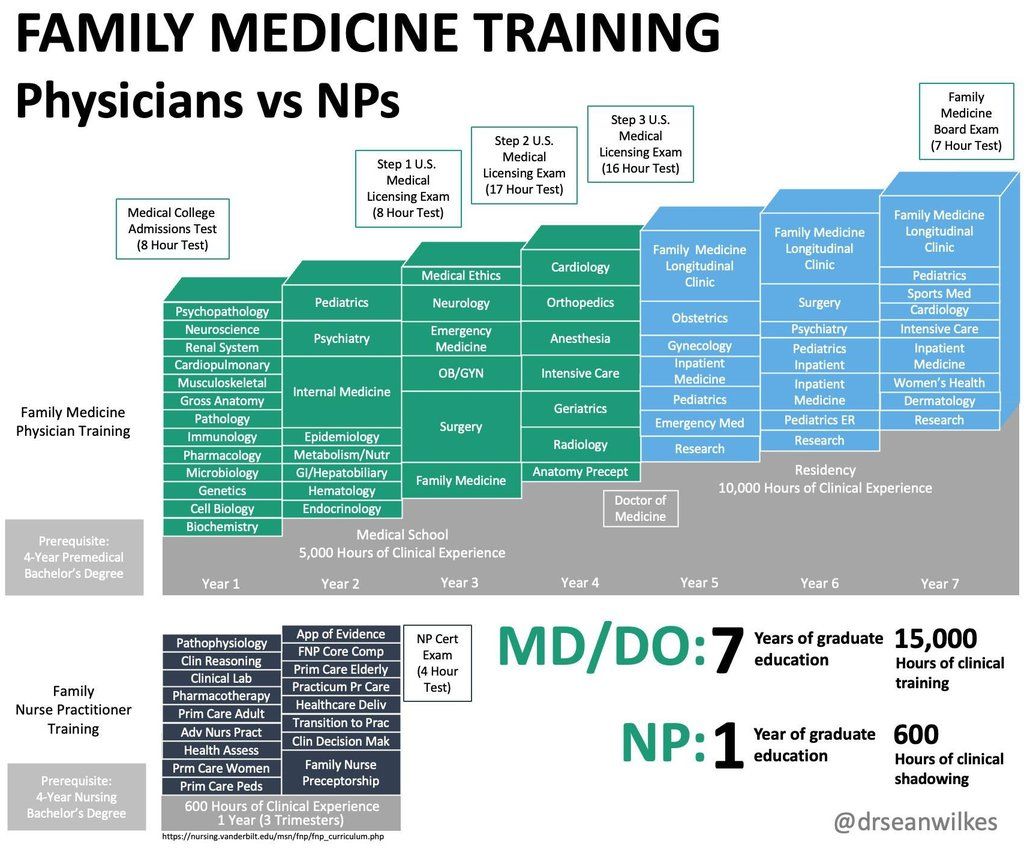
In recent times, both the American Association of Nurse Practitioners (AANP) and the American Academy of Physician Assistants (AAPA) have lobbied heavily for the ability of NPs and PAs to practice independently, free of physician oversight, as has traditionally been the case. Given the vast difference in educational rigor and clinical training hours between physicians and midlevels, it is no surprise that multiple studies comparing physician and midlevel practice have shown that physician-led care is associated with better patient outcomes, lower costs, and greater adherence to evidence-based practice.

In a hospital setting, patients are likely to encounter non-physician midlevel providers nurse practitioners (NPs), physician assistants (PAs), and nurse anesthetists (CRNAs, or Certified Registered Nurse Anesthetists). In the interest of political correctness, many institutions now prefer to use terms such as "advanced practice provider" (APP) or "physician extender" to refer to these various flavors of midlevel providers, an alarming trend that has been embraced by midlevel societies such as the AANP and AAPA. In 2021, the AAPA began a public relations effort to rebrand physician assistants as "physician associates". In addition, many institutions have simply resorted to using the word "provider" as an all-encompassing term that includes physicians as well as the aforementioned non-physicians such as NPs and PAs. The use of these ambiguous and nebulous terms creates confusion for patients, blurs the lines between different members of the health care team, and worst of all, attempts to establish a false equivalency between the inherent hierarchy of residency-trained, board-eligible/board-certified physicians and midlevel providers who may only have an online degree and a few hundred hours of unstructured clinical training and exposure.
With these facts in mind, MidlevelWTF aims to aggregate and publish content that documents and exposes real-world, concrete examples of midlevel malpractice, misconduct, and clinical ignorance in order to show why allowing midlevels to practice independently without physician leadership and close oversight is bad patients and doctors alike. Don't get us wrong - our goal is not to indiscriminately attack midlevel providers. On the contrary, we support the use of properly-supervised, well-educated midlevel providers as a part of physician-led healthcare teams. The dangers of unsupervised medical care by midlevel providers and the critical importance of maintaining physician supervision and leadership in healthcare is explored in much more detail in the book Patients at Risk: The Rise of the Nurse Practitioner and Physician Assistant in Healthcare, by Niran Al-Agba, MD and Rebekah Bernard, MD.


Who are you?
MidlevelWTF is the brainchild of a cadre of physicians concerned about the steady decline of the US healthcare system, caused in no small part by the prioritization of profits over patient care and the proliferation of poorly-supervised or completely unsupervised midlevels across the healthcare spectrum, from large hospitals to small clinics.
MidlevelWTF is not affiliated with or endorsed by Physicians for Patient Protection. However, we strongly support the excellent work they do to advocate for physician-led, physician-supervised care!
Press Mentions
- Jeanne Pinder. (2023, November 21). Nevada liposuction brings medical complaints. Clear Health Costs. https://clearhealthcosts.com/blog/2023/11/nevada-liposuction-brings-medical-complaints/
- Douglas Farrago, MD. (2023, September 3). Let’s Outsource Psychiatric Services to NPs. Authentic Medicine. https://authenticmedicine.com/2023/09/lets-outsource-psychiatric-services-to-nps/
- Clare Xanthos, PhD. (2023, April 8). When Prejudiced Providers Show Their True Colors. https://clarexanthos.medium.com/when-prejudiced-providers-show-their-true-colors-b8865378615f
- Todd Shryock. (2022, December 2). The NP training debate. Physicians Practice. https://www.physicianspractice.com/view/the-np-training-debate
- Tinker Ready. (2021, June 2). NPs and PAs Performing Colonoscopies: Why Not? Medscape Medical News. https://www.medscape.com/viewarticle/952284
