NP just feels like insulin shouldn't be started yet
💬 0 comments
Starting a patient like this on metformin is like pissing into the wind.
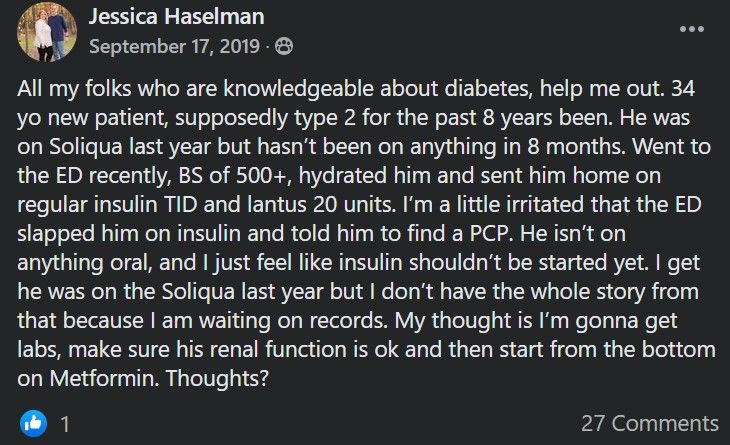
Wow, it sounds like the emergency department really rustled this nurse practitioner's jimmies! How DARE they start a patient with a blood glucose of more than 500 on insulin and tell him to find a PCP! NP Jessica Haselman is irritated that this patient wasn't started on any oral antihyperglycemics - DKA or HHS be damned! After all, why would a patient who already has history of insulin-dependent type 2 diabetes and was previously on Soliqua possibly need insulin? Oh, and you're going to get labs and "make sure his renal function is OK"? What do you think the ER physicians were doing when this patient was there? And "start from the bottom on metformin"? What do you think this guy's A1C is, with a random blood glucose of more than 500? This midlevel's clinical judgment and medical decision-making (or lack thereof) is truly a work of art. You might as well try moving a jumbo-sized container ship stuck in the Suez Canal with a single excavator. Oops, too soon?

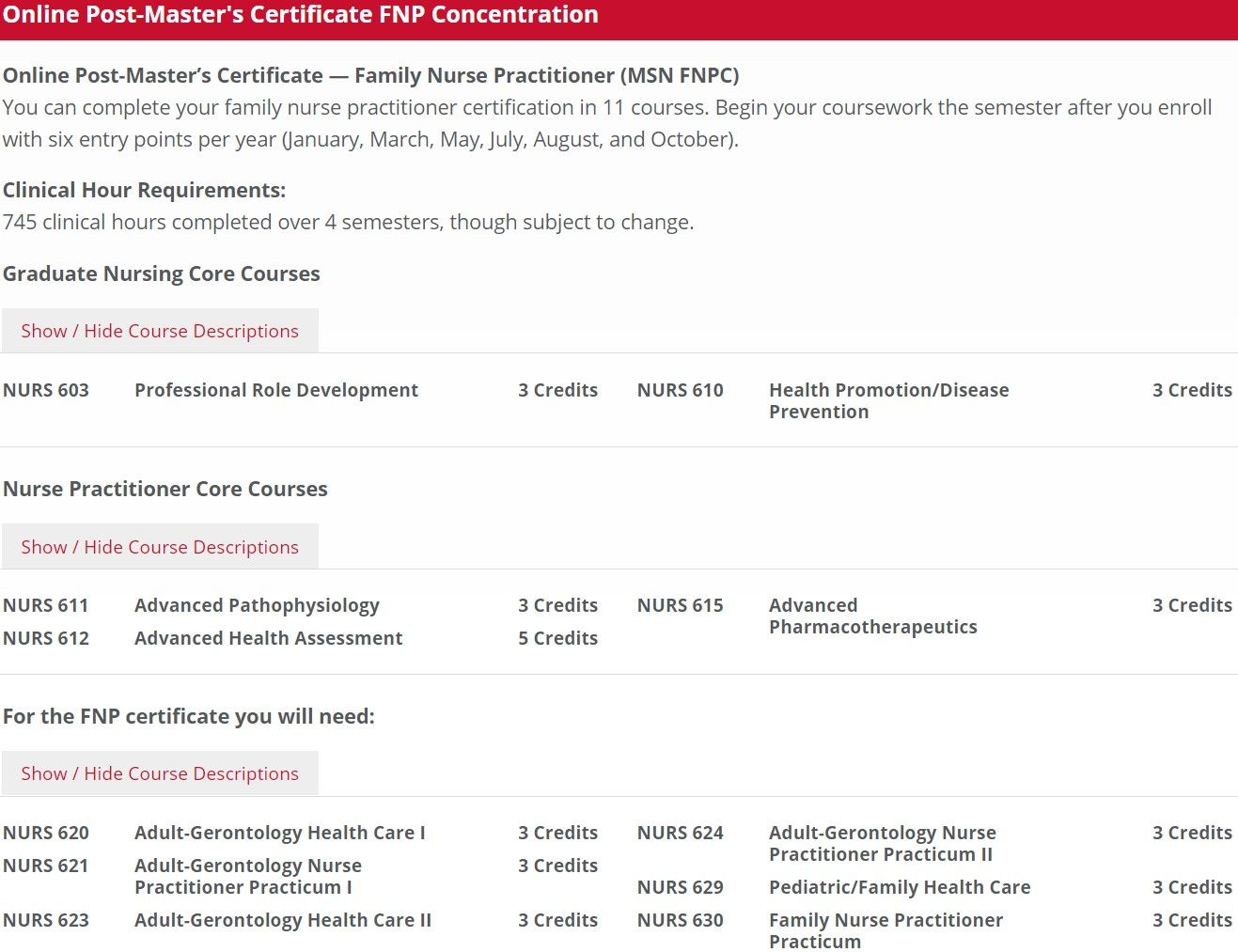
Diabetes diagnosis and management is considered bread-and-butter for any internal medicine or family medicine physician. Hell, we'd wager that a third or fourth-year medical student could make decent headway in formulating an appropriate initial management for diabetes just by using reputable clinical references (hint: consulting other randoms on Facebook is not considered a reputable reference source.) Apparently, this isn't the case for nurse practitioners, particularly ones who graduate from the Maryville University online FNP program. What exactly do they teach in "Advanced pharmacotherapeutics" and "Adult-Gerontology Health Care", we wonder? Nothing as advanced as when to use insulin to fucking treat diabetes, evidently! And wow, 745 clinical hours. That's like, 100-200 hours more than your average NP program! It really makes you think about what exactly they're doing during that time - probably nothing productive, when a third-year medical student could've completed an entire four-week internal medicine clerkship, passed the shelf exam, and learned enough about basic diabetes management in the process to put almost any midlevel to shame. And needless to say, any medical student who tries to take Step 2/3 of the USMLE without knowing cold the basic A1C targets for antihyperglycemic therapy and the various classes of insulin and oral antihyperglycemic agents is gonna have a bad time.
We wonder how this patient is doing today. Hopefully, this midlevel didn't decide to "start from the bottom". People with diabetes deserve healthcare professionals with top-end knowledge, training, and experience - and that means seeing a physician, not a midlevel.