The latest from the AANA propaganda desk: CRNA Education
💬 0 comments
Whoever makes these AANA infographics needs to lay off the ketamine and coke.

Last December, the American Association of Nurse Anesthetists (we do not recognize the legitimacy of their name change to the American Association of Nurse Anesthesiology) released the following infographic to "educate" the masses on CRNA education. Ironically subtitled "The Spin vs the Facts", it's clear to anyone with more than a couple of brain cells to rub together that the real spin-master here is no one else but the AANA.
The AANA attempts to cajole us with a handy-dandy bar chart comparing the training of a CRNA with that of a physician anesthesiologist. How fucking audacious of them to try to equate an undergraduate nursing degree (i.e. a BSN) to a graduate-level MD/DO medical degree. Did they conveniently forget to mention that prior to hurdling the single-digit acceptance rates to medical school, pre-med hopefuls are also required to ace a four-year undergraduate degree, traditionally in a science-based field such as biology or biochemistry, and earn a competitive score on the grueling 7.5-hour exam that is the MCAT?


Meanwhile, don't even get us started on how much of a complete joke nursing school is in terms of admissions requirements. Do you know what it's called when someone with a 2.5 GPA or an ACT score of 23 pays the fee to submit their medical school application? Making a donation. And we haven't even begun to scratch the surface when it comes to the countless numbers of online diploma mills offering associate's-to-BSN programs with admissions criteria even looser than your mom's genitals as described by the 12-year old kid on Xbox Live. By the way, AANA, may we suggest that you also add K-12 grade school to your CRNA education chart?

As for the academic rigor (or complete lack thereof) of an undergraduate nursing program, it's no secret that the difficulty of nursing school is essentially nonexistent compared to that of medical school. If medical school were an 80-proof vodka, nursing school would be a root beer. Don't believe us? Try sticking a fresh BSN student in a first-semester medical school biochemistry class and see if they're still alive after the first couple of weeks. And don't even get us started on the difference between standardized tests, e.g. the NCLEX versus the USMLE.
The AANA also tries to pull the wool over our eyes by labeling the CRNA as a "doctorate" degree. While it is true that more and more CRNA programs are "migrating" (inflating?) to a "Doctor of Nursing Practice" / "Doctor of Nurse Anesthesia Practice" model, the CRNA degree has traditionally been recognized at the master's level, and indeed, quite a few CRNA programs continue to offer MS/MSN degrees. In any case, trying to compare CRNA training with anesthesiology residency is a fool's errand at best. Try asking a CA-2 anesthesiology resident (or better yet, an intern stuck on the medical floors) if the SRNAs work harder or longer than they do, and you'd get laughed out of the hospital so fast that the CRNAs won't even have time to take their mandatory lunch breaks. Indeed, we can attest firsthand from our own experiences in residency that the SRNAs along with their supervising CRNAs would always be the first to leave for the day and the first to take breaks, forcing the anesthesiology residents to cover for them and clean up their afternoon messes. And by no means is this an isolated experience.
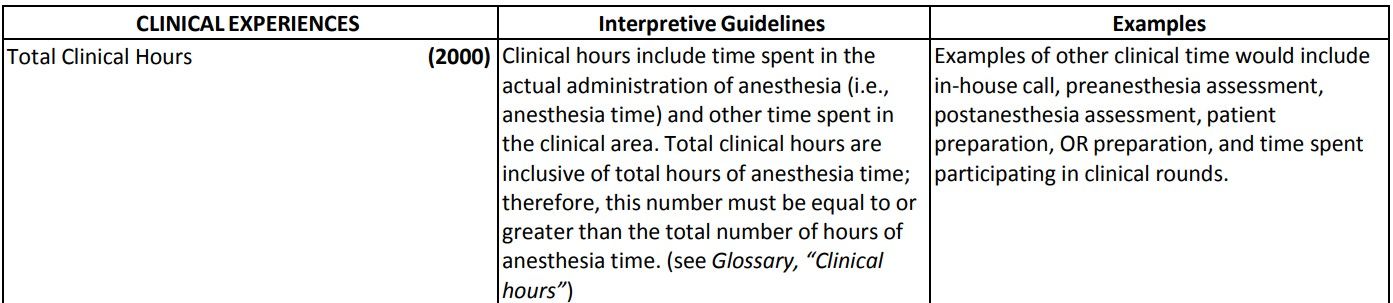

We're also not sure which ass the AANA pulled the "CRNAs have an average of 12,593 hours of clinical experience" from. Are they counting classroom time? Time spent as a nurse? We have it on good authority, including from the Council on Accreditation of Nurse Anesthesia Educational Programs itself, that the number is more like 2,000 hours - a far cry from the 10,000-15,000 hours (or more) of clinical training, often in 80-hour weeks, that an attending anesthesiologist will have accumulated through a year of general internship (PGY-1), three years of anesthesiology residency (CA2-4), and possibly fellowship in subspecialties such as critical care, pain management, transplant anesthesiology, etc. Seriously, since when did you see a SRNA or CRNA spend 80 hours a week at work? It is no exaggeration to conclude that the education of an anesthesiologist blows that of a midlevel CRNA out of the water.
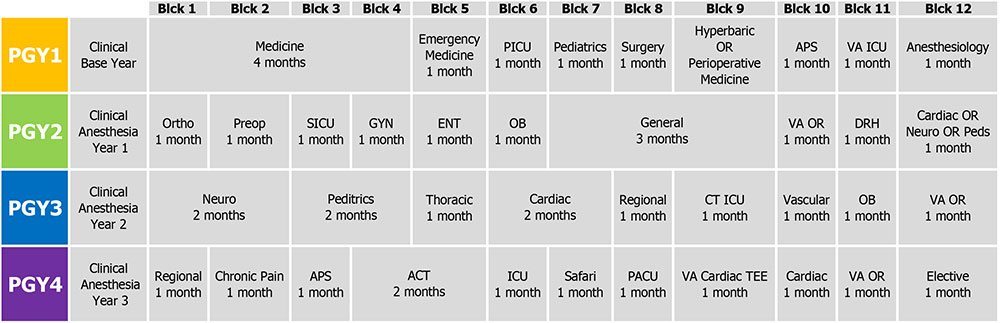
You know the AANA is increasingly desperate and grasping for straws when they have to resort to preposterous claims like "Unlike physician anesthesiologists, CRNAs are required to have critical care experience before they begin their anesthesia education". What in the actual fuck? Did they forget about the EM, ICU and pulmonary medicine rotations in medical school? Or the fact that virtually every anesthesiology resident will have rotated in the ICU during intern year? And that they will continue to have several more months of ICU time as an anesthesiology resident? Most importantly, do they really believe with a straight face that a couple years' stint as an ICU nurse really counts as "critical care experience"? You want real critical care experience? Then go to medical school, complete an IM/EM/anesthesiology/surgery residency, and then apply for a critical care fellowship. The AANA doesn't have the faintest idea what "highly educated" and "expertly trained" means, and it shows.

Speaking of fellowship, we were intrigued by the AANA's claim that CRNAs "pursue additional years of education in their specialty through fellowships". While there is no shortage of well-established fellowship programs for physicians, we've never heard of CRNA fellowships, and we've definitely never met a CRNA who expressed interest in further training - after all, the midlevel educational model is built around the idea of taking shortcuts. What fellowships do they speak of? Well, it turns out that there's a list, and assuming you haven't had any fingers amputated, you can count the list of accredited CRNA fellowships on one hand, because there's a whopping five of them. Hooray!


The AANA loves to accuse "physician special-interest groups" (are they referring to Physicians for Patient Protection?) of using scare tactics, but as our comprehensive takedown shows, there's no getting around the cold, hard, fact that physician anesthesiologists are better-educated and better-trained than midlevel CRNAs, and by no small margin. We hate that we even have to use the term "physician anesthesiologist". Indeed, if it weren't for the AANA's politically motivated push to rebrand nurse anesthetists as "nurse anesthesiologists" and rename their organization accordingly - a move that was universally condemned by the American Society of Anesthesiologists and cock-blocked by the New Hampshire Supreme Court - making such a distinction would be wholly unnecessary. But, alas, such is the reality of the never-ending war between physicians and midlevel providers looking for shortcuts to power and money. As the old adage goes, everyone wants to be a doctor, but no one wants to go to medical school.